Your Trusted Virtual Assistant Partner for USA Healthcare
Streamline operations, reduce admin burden & increase patient satisfaction — with expert virtual support tailored for healthcare.
How does it work?
Our process is straightforward: we’ll start with a quick audit to understand where our support will be most effective. Then, we’ll share profiles of virtual assistants from our database that match your needs. Once you choose, we’ll handle the onboarding process seamlessly, respecting all your existing protocols. Our charges only begin once your assistant is fully prepared and ready to go. At KVRS, we’re committed to easing your workload and simplifying your day. It’s that simple!

Healthcare Virtual Assistants
Help co-ordinate appointments with patients, data-entry and insurance filing. Optimize your practice by delegating scheduling, call management, and administrative tasks to our expert healthcare virtual assistants.
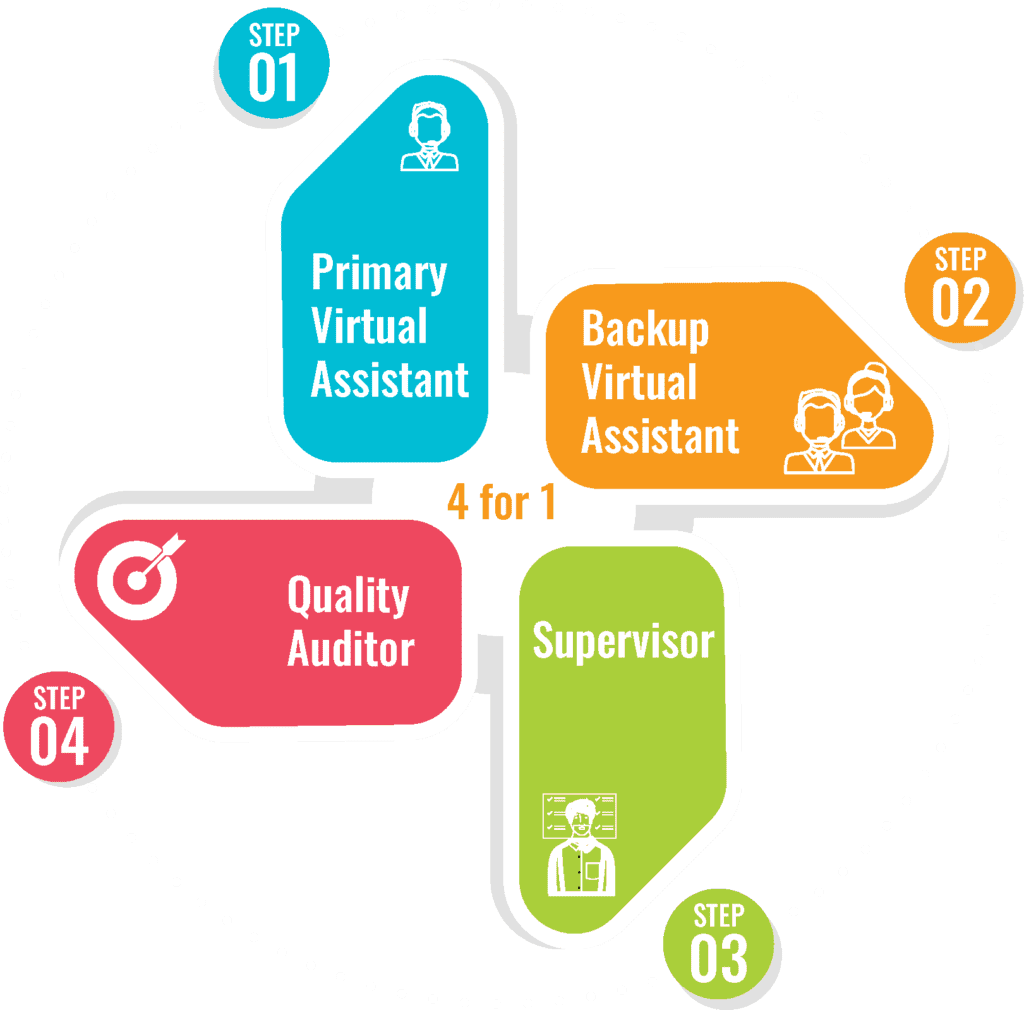
Maximize Healthcare Support with Our 4-in-1 Virtual Medical Assistant Service
Ensure seamless operations with a Backup Virtual Assistant, included at no extra cost in most plans. Daily oversight and support from experienced supervisors are also provided, along with quality audits conducted by a dedicated Quality Auditor.
With KVRS, you pay for a primary Virtual Assistant but also receive:
- A Backup Virtual Medical Assistant
- A Supervisor for guidance
- A Quality Auditor for performance checks
KVRS offers a comprehensive 4-in-1 Virtual Medical Service, helping healthcare organizations streamline operations, reduce costs, and maintain high-quality service. Our commitment to excellence ensures you can focus on delivering exceptional patient care.
Medical Virtual Assistant Services
Appointment Scheduling
At KVRS, we streamline patient appointment scheduling to reduce no-shows, optimize clinic workflow, and enhance daily operational efficiency.
Data Entry Services
Our accurate and timely medical data entry services keep your EMR and patient records organized, updated, and compliant with industry standards.
Insurance Verification & Eligibility
We provide fast and precise insurance eligibility verification to prevent claim errors and reduce rejections, ensuring a smooth billing workflow for your practice.
Billing & Insurance Services
KVRS delivers complete medical billing and insurance claim management, helping practices reduce denials and secure timely reimbursements to strengthen their revenue cycle.
Administrative Support
We handle routine administrative tasks so healthcare providers can focus on delivering quality patient care. KVRS offers dependable virtual administrative support for clinics and medical practices.
Prior Authorizations
Our team manages prior authorizations efficiently, ensuring faster approvals and seamless continuity of patient care.
Our Simple 3-Step Onboarding Process

Consultation & Needs Analysis
We discuss your practice, pain points, workflow, and compliance demands.
Custom Setup & Training
We deploy assistants, train them on your systems & protocols, and integrate.
Ongoing Support & Optimization
Continuous monitoring, feedback, process improvements, and reporting.
Discover How KVRS can Ease your Workload and Simplify your Practice
Full-Time Virtual Assistants
Clients can opt for a dedicated FTE to ensure consistent service over time. Enjoy the comfort of hearing a familiar voice daily, knowing you can rely on a professional who delivers expert results. They’ll adapt to your workflow and integrate seamlessly with your office staff.
Part-Time Virtual Assistants
We can provide a fully trained virtual assistant to manage absenteeism or assist on busy days.
Why Healthcare Providers Choose KVRS

Get Started in just 1 Hour
Only 1 hour of onboarding training is needed to go live. Enjoy a seamless experience with the support of a dedicated onboarding manager throughout the process.

No Long-Term Commitment
No long-term contracts required – you can cancel anytime. Choose the hours you need and adjust them based on demand.

Save 70% on Costs
Pay only for the services you use – no charge for absences such as vacation or sick days.
Multifunctional Roles
Our VAs are skilled in a wide range of tasks, including appointment scheduling, confirming appointments, charge posting, billing. Choose the specific skills your business needs.

Round-the-Clock Availability
KVRS virtual assistants are available to manage your patients' needs, even beyond US regular office hours.

EHR/EMR Adaptability
Our virtual assistants are trained to effortlessly navigate any EHR/EMR system, providing seamless integration to enhance flexibility and efficiency in your healthcare operations.
Skilled in Leading EHR and PACS Systems
The modern world is in a continuous movement and people everywhere are looking for quick.












KVRS LITE
This plan includes the following
- Parsing Emails / Faxes
- Appointment Scheduling
- Appointment Reminder
- Updating Patient Files
- Patient / Referral Coordination
KVRS ESSENTIAL
Everything from KVRS Lite plus
- Online / Live Scheduling
- Outbound / Inbound Calls
- Voicemail Support
- Multi-language SMS for Patients
- Daily Analytic Report
KVRS PREMIUM
Everything from KVRS Essential plus
- White glove setup
- Benefits & Eligibility Verification
- Prior Authorization
- Denial Management
Client Testimonials
Zachary Elgart
Adding virtual assistants to our diagnostic radiology front office operations has been easy, quick and cost-effective. The virtual assistants schedule the patients, inform and confirm the patients appointments as well as answer any patient queries. Knowing that assigned tasks are done and done on time and executed correctly is worth every penny. KVRS has really been awesome.
Zachary Elgart
Allegiance Radiology
Bradford Ames
Finding good candidates to obtain authorizations for CT and MRI referrals is not an easy task. KVRS showed us, that the time we could spend on recruiting and training in-house, can be substituted by highly trained KVRS agents, and the long-term goals would be much more profitable and less stressful.
Bradford Ames
ImageLink
David Mildenberg
We spent 2 days training the virtual assistants for claim scrubbing processes. Now we can fully rely on our virtual assistants to prepare error free claims for submission to the insurance carriers. we are very pleased with KVRS’s Service.
David Mildenberg
RevEx
Frequently Asked Questions
Who are your Virtual Assistants?
Our virtual assistants go through a thorough application and interview process. They are carefully selected for their skills to work in a remote medical setting.
What kind of tasks can a Virtual Assistant handle?
Our virtual assistants can help with tasks like live charting, transcription, office work, phone calls, and more. If it’s something that can be done on a computer, our VAs can likely handle it. They can assist with referrals, refill requests, faxing, phone calls, insurance checks, prior authorizations, eligibility, calling patients or insurance companies, and much more.
What is the role of denial management?
Denial management refers to the process of identifying and resolving claims denials from insurance companies or other payers. The role of denial management is to minimize the impact of denials on revenue by identifying and resolving the root causes of denials, such as coding errors, incomplete documentation, or incorrect patient information.
What are the types of denials?
Denials can be classified into two main categories: hard denials and soft denials. Hard denials are denials that cannot be appealed and require corrective action, while soft denials are denials that can be corrected and resubmitted.
What are the 5 denials?
- Duplicate claim/service
- Service not covered by payer
- Service not medically necessary
- Incorrect coding
- Missing or invalid information
What does AR followup mean?
AR follow-up (Accounts Receivable follow-up) refers to the process of contacting insurance companies or other payers to inquire about the status of outstanding claims that have not been paid or have been partially paid. The goal of AR follow-up is to identify any issues or reasons for the delay in payment, such as missing information or errors in coding, and to take corrective action to ensure that the claims are paid in a timely manner. AR follow-up is a critical component of revenue cycle management in healthcare, as it helps ensure that healthcare providers are reimbursed for the services they provide.
What are the roles and responsibilities of RCM?
What Is a Revenue Cycle Manager? As a revenue cycle manager, you manage patient billing and insurance claims for a medical facility. Your job duties include creating reports, analyzing data, identifying lost revenue, collecting payments, and implementing revenue cycle management (RCM) strategies to minimize losses
How much does revenue cycle management services cost?
Every organization wants to be appraised of the cost of integrating revenue cycle management services. This is helps you to better understand the cost impact on your organization. It is important to note that the cost impact will be different in each case. For instance, it will be dependent on the number of patients you serve, the different insurers you’ll be dealing with and your amount of patient encounters.
What is the role of a remote assistant in healthcare?
In this remote position, your responsibilities include entering patient data into files, maintaining a database of records, scheduling appointments for patients, and collecting information for patient health assessments online or over the phone.
What are the six stages of the revenue cycle?
Step 1: Patient Pre-authorization
Step 2: Eligibility & Benefits Verification
Step 3: Claims Submission
Step 4: Payment Posting
Step 5: Claim Denial Management
Step 6: Reporting
Contact Us
Feel free to fill out the form below to get in touch with us.
USA Office:
- Address: 2609 Crest Valley Drive, Conyers,
- GA-30094, USA.
- Phone: +1 470-993-2442
- Email: info@kvrsvirtualassistant.com
India Office:
- Address: 1 Bijal Apartment, Near Hari Nagar,
- Gotri, Vadodara-390021, Gujarat, India.
- Phone: +91 799 066 4280
- Email: info@kvrs.co.in
